Sussan Ley updates the nation on Medicare
As any regular reader of my work is aware, I have been very vocal about the various changes to Medicare proposed by the LNP government. A list of past articles is provided at the end of this article should you have missed out. I also appeared on the ABC News supporting the RACGP in their “You’ve Been Targeted” campaign.
Earlier this week I wondered what was happening. Minister Ley had promised to consult with doctors before making any changes. I’d suggested Ley not forget about the most important demographic: the patients. I Googled and didn’t find much. I checked Ley’s Twitter feed and found the odd tweet about consulting with doctors.
https://twitter.com/MalBrough_MP/status/563504992078688257
Meeting with doctors and
Impressed with the integrated model of care at Launceston Medical Centre- GPs, specialists, skin clinic and more pic.twitter.com/pHLScmZtJ8
— Sussan Ley (@sussanley) February 15, 2015
more doctors.
Where are the meetings with PATIENTS? This one, maybe?
With @andrewnikolic @brettwhiteleymp in Northern Tasmania – Talks on how best to protect Medicare for the long-term. pic.twitter.com/LvhGWmfdYQ
— Sussan Ley (@sussanley) February 13, 2015
Possibly, but they look suspiciously like more medicos to me. I was becoming a little depressed. Yesterday Ley finally held a press conference. The full transcript is available: Update on nationwide Medicare policy consultation.
Craig Laundy: It’s great to have the Health Minister, the Honorable Sussan Ley and my good friend the Member for Lyne Dr David Gillespie here in Reid for an afternoon of consulting with local GPs so without further ado Sussan welcome.
Not one word about PATIENTS! More doctors! Yes, doctors are voters, just like you or I. Yes, doctors pay the Medicare levy just like you or I. Yes, doctors have a vital voice in any changes to Medicare. You and I have a far greater voice and we must not let Ley forget that.
I’ve just come from breakfast this morning on the Central Coast. There were 40 doctors and lots of different views in the room and the same for last night and I’m on my way to another part of the country to do something similar.
Still no mention of PATIENTS. *sigh*
…accept that unless you’re in a vulnerable category maybe those services don’t come absolutely for free and that where there is an ability to pay that you value the high quality service that you receive that you do indeed pay something. When I look at the number of bulk-billed consultations across the country 76 per cent of all episodes of care are bulk-billed to non-concessional patients.
No, Ley, any bulk-billed service to a non-concessional patient is certainly not for “absolutely free” as most non-concessional patients are working and paying the Medicare Levy! Or are the children of people paying the Medicare Levy. That’s not “free”, we pay an insurance premium. I’ve heard it said there are medical practices that bulk-bill 100% of their consultations. I’ve yet to actually attend one, but I have no doubt there are some. There are also practices that bulk-bill only those holding a Health Care Card.
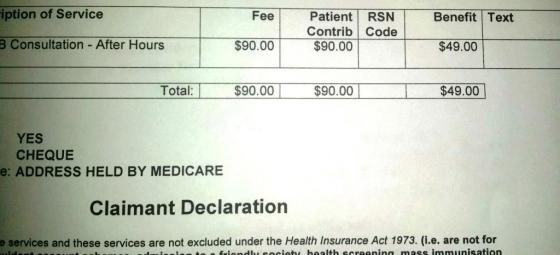
The practice I go to has a policy of bulk-billing walk-ins (see first available doctor) between 7 am and 6 pm. Appointments are not bulk-billed, nor are consultations after 6 pm or on weekends or public holidays. I think there are many practices with similar policies. How often am I a walk-in? Not too often. I work full-time and also have medical conditions which I prefer to have overseen by a regular doctor. Consequently most of my consultations are either by appointment or outside of the bulk-bill hours, even if I am walking in with a child that needs a stitch in a toe – no appointment, but 8 pm at night. $90 payment, $49 rebate. My co-payment is already $41, thank you very much. The average patient contribution for out-of-hospital services for patients who pay is $51 (including specialists visits).
I wanted to see proof of this 76%. I thought the annual report might be a good place to start, but as Medicare has been absorbed into the Department of Human Services, there doesn’t seem to be much Medicare detail in that report. The Department of Human Services ended the 2013-14 year with an operating SURPLUS.
In 2013–14 the department administered an estimated $159.2 billion in payments or around 38 per cent of government outlays. Financial performance targets were met, for the most part, and the department reported an operating surplus of $132.6 million after adjustment for unfunded depreciation and the revaluation of assets. This compares with a deficit of $7.7 million in 2012–13.
Source: Department of Human Services Annual Report
That doesn’t tell me anything about bulk-billing though, interesting as the information may be. Further research found bulk-billing statistics. Click the image to go to the full table. According to the Medicare statistics, 77.2% of consultations were bulk-billed for the 2013-14 year, but there are vast differences across services. GP visits are bulk-billed 82.2% of the time, whereas specialists a mere 29.2%. No clear differentiation is given in the report between concessional and non-concessional patients, so are we to assume only 1.2% of consultations were for concessional patients?
Clearly doctors in Canberra don’t believe in bulk-billing politicians.
I am struggling to believe the rate is this high. If you want to delve into the full statistics yourself, the spreadsheet available is very useful.
Why is the rate of bulk-billing so high? Based on my own personal experience and that of friends, family and co-workers, my guess would have been less than 50%. The history of Medicare may have something to do with it. I found this interesting snippet. Read very carefully.
Levels of bulk billing for unreferred GP attendances have been declining in recent years after reaching a high of 79.7 per cent in1996-97. By the December quarter 2002 bulk billing for unreferred GP attendances had declined to 68.8 per cent, but by June 2004 this had improved to 70.2 percent.
Source: APH
The decline in bulk-billing had been viewed as a negative! Incentives of $7.50 to encourage doctors to bulk-bill were introduced in 2004.
From 1 May a $7.50 incentive paid to GPs for bulk-billed GP consultations with concession card holders and children under 16 in non-metropolitan areas (RRMAs 3-7) and Tasmania introduced. This incentive replaces the earlier $5 incentive in these areas.
As of 1 September eligibility for the $7.50 incentive payment to GPs extended to eligible urban areas and large regional centres.
Clearly bulk-billing was encouraged in more ways than one.
Between 1992 and 2003 the Scheduled Fee rose 26%. The CPI rose 31%. Doctors were taking a pay cut.
Interestingly, during the 2004 election campaign, the Coalition proposed to increase the rebate to 100% of the scheduled fee. Different captain at the same helm eleven (eleventy?) years later wants to cut the rebate.
Proposals for changes to Medicare were announced by the Coalition during the 2004 election campaign. These include from 1 January 2005 increasing the Medicare rebate for all GP services to 100 per cent of the Schedule fee…
Source: APH Library Archive
When did the big clinics emerge? Edelsten opened the first after Medicare came into being in 1984. We now have very professional corporate medical businesses, minus the chandeliers and gawdy trimmings.
Reading through the history, it is clear Medicare has been tweaked many times over the years. The practice of medicine has evolved. We no longer visit our local family doctor in the front room of his residence as in days gone by. The economies of scale from multi-disciplinary and multi-doctor practices would, I think, be necessary in circumstances where fee increases were running well behind CPI increases AND bulk-billing was being encouraged.
The HICAPS system has been a great innovation. The doctor gets paid at the time of service and the patient receives the rebate overnight in their bank account. As noted in the past, I’ve actually received the rebate credit before the payment debit hit my bank account. For patients this saves considerable time. In the last twelve months I’ve only visited one medical provider (and we know I’ve visited a few) that had not yet moved to HICAPS. Gone are the days of lining up in a Medicare office to claim medical bills.
The medical profession was initially resistant to Medicare. The medical profession today is a very different beast to the medical profession of forty years ago. Many practitioners are not as politically right wing as their predecessors. Free university education saw many from different backgrounds obtain degrees.
Forty years is a long time. You may be reading this on a smartphone. Medicare was launched three years before Telstra launched the first mass mobile network in Australia.The phone cost $5,200. Technology, medicine, society: all have changed.
How much revenue does the Medicare Levy raise? That seems to be the greatest secret, as despite considerable research, I can’t find the answer. The spreadsheet I referred to above analyses the costs of Medicare to the nth degree, sliced and diced to within an inch of the core and tells me the benefits paid were $19.1 billion. Not a revenue number in sight. Nor, for that matter the infrastructure, staff and other costs (such as HICAPS).
Was Medicare ever intended to be completely self-funding?
The objectives of the original Medibank were summarised by R. B. Scotton (1977) as universal in coverage, equitable in distribution of costs, and administratively simple to manage.
That statement doesn’t really specify self-funding. As it turns out, the original funding bills weren’t passed and the funding came from general revenue. The levy came later.
“Equitable in distribution of costs” doesn’t mean the same thing as self-funding. In any case, what was appropriate forty years ago may not be appropriate today – and that could be either way. How do we assess “equitable”? These are social questions, not medical questions, yet I see Ley focussing on the medical profession and not the people.
To be continued . . .
Previous Medicare related articles by the author:
- How much does it cost to COMPLETELY collect and process that $7?
- You’ve been targeted: supporting the AMA and RACGP supporting us
- How Medicare Rebate cuts may impact the patient, other than cost
- In the Australia of the future, you will fly out to see a doctor
- Medicare is YOUR insurance cover
- What is this premature performance costing the taxpayer?
- Open Letter to Sussan Ley on Medicare changes
- The growth of Medicare is slowing
This is a slightly edited version of the article originally published on Love versus Goliath









26 comments
Login here Register here-
stephentardrew -
Meryl -
Meryl -
paul walter -
Florence nee Fedup -
Robyn Oyeniyi -
jagman48 -
Kaye Lee -
Robyn Oyeniyi -
Kerri -
Meryl -
Team Oyeniyi -
John Fraser -
John Fraser -
Margaret McMillan -
Ricardo29 -
Florence nee Fedup -
Loz -
Mike -
Robyn Oyeniyi -
Matters Not -
Michael Taylor -
townsvilleblog -
olddavey -
-
LOVO
Return to home pageThanks Robyn very informative.
Walk ins without appointments how is that possible, I have to make an appointment two weeks in advance and then they always keep me waiting for at least an hour and a half.
What planet do these Liberals live on a treasurer who has never filled in a tax form and can’t count and a Health minister who doesn’t understand we pay for medical services through our medicare levy.
I’d say a lot of change comes down to panelbeating our more use-value system into something Americanised.
I can’t thnk of too much that has been changed this century that has been designed with people in mind, apart from bankers and ideologues,
Ley is also not talking to others in the health industry. Doctors are only a small part of the industry.
Florence, most pathology and imaging services are also bulk-billed – I’d like to know is Ley planning to change all of that as well? My imaging bill one day was $951. These costs can be expensive.
Why can’t we find out what the medicare levy brings into the Government. Surely it must do something to the cost of the service to them ?
jagman,
This is about two years old (May 2013)
The changes to the Medicare levy (from 1.5% to 2%) are expected to raise $20.4 billion between 2014-15 and 2018-19, when the full scheme comes into place. But with the total cost of the NDIS estimated at $8 billion a year, the levy won’t come close to fully funding the scheme. The Medicare levy (including the surcharge) raises around $9 billion a year; Medicare costs over $17 billion.
Thanks Kaye Lee and yes, I have now been passed other revenue sources from a kind reader. I would have expected the figures to be available in the same spreadsheet as the costs information! Silly me! 🙂
Good to have more than one source.
I find the figures we are constantly being told around the payouts from Medicare somewhat spurious. I have numerous medical complaints that involve my GP and at least 6 specialists. I also have regular Gastroscopy, colonoscopy, bone densitometry, breastscreen, mammogram and ultrasounds. My husband doesn’t see specialists so much but visits the GP often for blood pressure and cholesterol issues. I have 2 daughters. One epileptic the other asthmatic and they each have other complaints such as Psoriasis and arthritis. In the last 5 years we have each been operated on. Some of us twice! Apart from the occasional x-ray or breastscreen I have only ever encountered bulk billing when my daughter’s alopecia required treatment twice a week. As each laser treatment took 2 minutes the dermatologist chose to bulk bill as the paperwork would take up more time than the actual treatment like 10 fold! I seriously wonder who these 80% are?? I know very few people, my pensioner parents included who are routinely bulk billed for everything! Do the 12 x2 minute treatments each count as equivalent to a 15 minute consult on these figures???
As for the alopecia treatment? Surely Sussan Ley would understand that a six week course involving 12 x 2 minute treatments would be ludicrous to co-pay! I would think she would have an understanding of that at least!
Yes Kerri I was bulk billed once at Mole Scan because I knew the doctor apart from that i have never been bulk billed, I have a very low income but don’t have a health card. I agree I don’t know many people who are bulk billed.
Kerri and Meryl, I am hearing many similar accounts. So far only one person has said they are consistently bulk-billed.
I would expect people to be telling me of much more bulk-billing.
It is indeed strange, but given the number of years of statistics available, it appears it must be correct!
The payouts I accept. It is the bulk-bill % I find unbelievable. But statistics never lie, do they? 🙂
<
I got the impression that Sussan Ley was walking a tightrope and was being very,very careful not to get caught in a lie.
Which must surely vex the pig Abbott.
Prepared to wait and see what she comes up with.
I note that the former Health Minister on the same day had a boat full of illegals sail straight through Australia's sovereign border.
http://www.smh.com.au/nsw/teenagers-eagle-eye-led-to-arrests-of-fugitives-paul-bennett-and-simone-wright-20150217-13h477.html
Once again Dutton fails ……. the wanker should get a bottle of black dye and start handing out $200 counselling vouchers.
<
Australian Skin Cancer Clinics are bulk billing here in Qld.
In Tasmania it is quite difficult to find a bulk-billing practice. The practice I attend decided about 2 years ago not to bulk-bill. However my own doctor after charging me once must have refused to toe the line and she always bulk-bills now (I’m a concession card holder).
I think those big bulk-billing practices only exist in the larger cities – at least that’s the only place I’ve ever seen them.
Stories like this are one of the reasons I really like the AIMN
Bulk billing was always meant to be universal. Doctors fought it in the beginning. it was NEVER meant to be safety net., I believe it allowed the government more power in keeping costs down.
Again the LNP are manipulating the figures saying that Medicare is unsustainable. Read Jeff Richardson, Professor and Foundation Director, Centre for Health Economics at Monash University, article in The Conversation headed 12 May 2014, 5.22am AEST
Australia’s ‘unsustainable’ health spending is a myth. There is nothing but lies coming from this government, and all to fit their ideology.
Doesn’t tobacco & alcohol taxes go towards medicare too
Loz, thanks for the tip. Interesting article and the analysis I did tonight produced results that are certainly not inconsistent with that article. I read the article after I’d done most of my number crunching and was heartened by the consistency. 🙂 I have lots of pretty graphs to share, which will be interesting for the number geeks amongst us, but others may feel their eyes glaze over if they are not into numbers.
John Fraser said:
Not quite true John. The Australian Skin Cancer Clinic at Chermside in Brisbane has about 5 doctors but only some of whom ‘bulk bill’. At least one other charges $70.00 for an initial consultation.
Not sure how the business model works.
Off for a visit this Thursday.
I’m lucky in my town – most clinics bulk bill. Quite a welcome change from the money grabbing doctors in Canberra.
Robyn, Of course the answer is a simple one, as it is in most things. The wealthy Australians who can well afford to pay more, should be made to pay more. We poor people are flat out putting food on the table, yet the multimillionaires and billionaires continuously avoid and evade paying their fair share of tax, if they did, we would not have a national debt, and further more we could afford all government agencies and services. However as long as people like Clive Palmer is in the position to buy his 15 year old daughter a $5 million yacht for her birthday, we will all continue to suffer.
Nikolic, a piece of human detritus if I ever saw one.
Pingback: Medicare is the wrong target February 22, 2015 Written by: Robyn Oyeniyi | winstonclose
Robyn, great story on my member Liar Ley (or Irrigators’ Ley-as some call her). I have met and talked with her many times. I once was impressed but as time has gone by I have become very, very unimpressed. She’s seems to be getting shonkier and shonkier… which may be why abbott made her an full minister because she’s an natural fit in his front bench of shonks.
I don’t think I have ever been to an Dr in ‘the Hill’ that doesn’t bulk bill. I have never had to pay…. ever…. and I work.
————————————————————————————————————————————————————————-
Townsvilleblog, not only may he have avoided paying tax, 😯 I seem to remember that he bought an mine from the Big Australian for 37mill. and claimed depreciation/etc and apparently got an 138mill. tax return that he said at the time ” it’s just beer money to me” 🙄